Sex reassignment surgery with Colon graft technique
Information on Colon Vaginoplasty
Overview of Colon Vaginoplasty
Colon vaginoplasty is a surgical procedure used to create or reconstruct a vaginal canal using a segment of the colon. This method can be utilized as an alternative to skin grafts during sex reassignment surgery (SRS) or as a corrective measure for patients who experience unsatisfactory vaginal depth post-SRS.
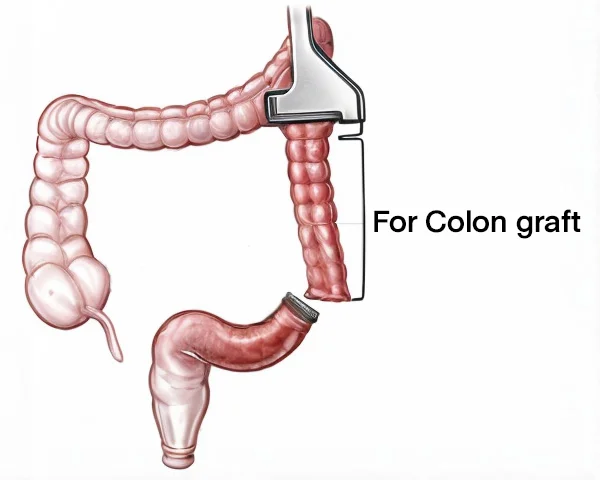
Surgical Technique
During colon vaginoplasty, a segment of the sigmoid colon (approximately 20 cm) is selected. One end of the colon graft is closed while the other end is left open and is slid through the vaginal tunnel to be sutured to the vaginal opening.
Indications for Colon Vaginoplasty
A: Primary Colon Vaginoplasty (Male to Female SRS with Colon Graft)
For primary sex reassignment surgery, Dr. Chettawut typically recommends the standard SRS (Non-penile inversion SRS with skin graft technique) over primary colon vaginoplasty to avoid potential abdominal complications. However, primary colon vaginoplasty may be considered in selective cases with the following criteria:
- Patients must be younger than 45 years old.
- Patients must weigh less than 80 kg.
- Patients’ BMI must be less than 28.
Related Topics:
- Concept of Non-Penile Inversion SRS
- Dr. Chettawut’s Non-Penile Inversion Technique
- Skin Graft Technique for Sex Reassignment Surgery
- Colon Graft Technique for Sex Reassignment Surgery
- Cosmetic Sex Reassignment Surgery Without a Functional Vagina
- Dr. Chettawut’s Recommendation of Genital Hair Removal
- Medical Care After Sex Reassignment Surgery
- How to Successfully Recover After Sex Reassignment Surgery
- Vaginal Dilation Routine After Sex Reassignment Surgery
- How to Prevent Possible Complications After SRS
B: Secondary Colon Vaginoplasty (Treating Short Vagina Post-SRS)
Secondary colon vaginoplasty is used to treat patients who suffer from a short vagina (vaginal depth less than 4 inches) or a collapsed vagina. The causes of these conditions can include insufficient creation of the vaginal tunnel during the primary SRS, poor healing due to skin graft failure, or lack of proper vaginal dilation.
Treatment Steps:
- Remove post-inflammatory scar tissue inside the vagina.
- Re-create the vaginal tunnel with proper dimensions.
- Use a colon graft to provide a new and healthy lining inside the vagina.
The colon graft is preferred over skin grafts in these cases because it brings its own blood supply, which aids in healing and provides self-lubrication.
C: Colon Vaginoplasty in Female Patients (Treating Congenital Absence of Vaginal Canal)
Colon vaginoplasty is also applicable to biological women suffering from congenital absence of the vaginal canal, known as Vaginal Agenesis, Mullerian Agenesis, or Mayer-Rokitansky-Küster-Hauser Syndrome (MRKH). This condition is characterized by the absence of the vaginal canal and uterus, while the ovaries remain intact.
Benefits of Colon Graft:
- Adequate lubrication
- Appropriate vaginal depth
- Short horizontal linear scar (like a C-section), as opposed to the unsightly scars left by skin graft harvesting
Conclusion
Colon vaginoplasty is a versatile and effective surgical technique for both transgender and cisgender women requiring vaginal reconstruction. Whether used as an initial procedure or as a corrective measure, the colon graft offers several benefits, including adequate depth, self-lubrication, and minimal scarring.
Contact Us
For more information or to schedule a consultation, please contact Dr. Chettawut’s office.
Dr. Chettawut’s recommendation program for Vaginal dilation routine
after Sex reassignment surgery with colon graft (Colon vaginoplasty)



